Melasma Solution
Who gets melasma?
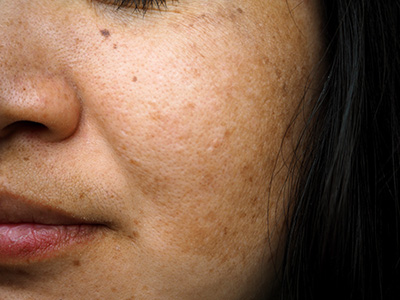 Melasma is typically common in women than in men; only 1-in-4 to 1-in-20 affected individuals are male, this depends on the population studied. It usually starts between the age of 20 and 40 years, but it can start right from the childhood while it may not start until middle age.
Melasma is typically common in women than in men; only 1-in-4 to 1-in-20 affected individuals are male, this depends on the population studied. It usually starts between the age of 20 and 40 years, but it can start right from the childhood while it may not start until middle age.
Melasma is a very common patchy brown, blue-grey or tan facial skin discoloration. It’s usually seen in women during the reproductive years. It normally appears on the upper lip, upper cheeks, chin and forehead of women between 20-50 years of age. It’s known to be primarily related to internal hormonal changes as seen in pregnancy and external such as birth control. It is also related to sun exposure.
What causes melasma?
Experts believe that the dark patches in melasma could be triggered by many factors which include birth control pills, pregnancy, family history of melasma, hormone replacement therapy (HRT and progesterone) and anti-seizure medications. Sunlight is the most important factor that causes melasma, especially in individuals with a genetic tendency to this condition.
The cause of melasma is complex. The pigmentation is caused by the overproduction of melanin by the pigment cells, melanocytes, which is taken up by the keratinocytes (epidermal melanosis) and/or deposited in the dermis (dermal melanosis, melanophages). There is a genetic predisposition to melasma, with at least one-third of patients reporting other family members to be affected. In most cases, melasma is a chronic disorder.
Fact about Melasma
- Melasma is most common in women 20-50 years of age.
- Melasma is caused partly by genetic predisposition, hormonal changes and sun.
- Melasma is characterized by three location patterns (cheekbone, jawline and central face).
- Melasma prevention requires sun avoidance and sun protection with sunscreen and hats.
- The condition is frequently treated with topical creams containing hydroquinone.

Things You Must Also Know
- Sun exposure and sun damage - this is the most important avoidable risk factor.
- Pregnancy - in affected women, the pigment often fades away few months after delivery.
- Hormone treatments - oral contraceptive pills containing oestrogen and/or progesterone, hormone replacement, intrauterine devices and implants are a factor in about a quarter of affected women.
- Certain medications (including new targeted therapies for cancer), scented or deodorant soaps, toiletries and cosmetics - these may cause a phototoxic reaction that triggers melasma, which may then persist for a long time.
- Hypothyroidism (low levels of circulating thyroid hormone).
Melasma usually arises in healthy, non-pregnant adults. Constant sun exposure causes deposition of pigment within the dermis, and this often persists long-term. Exposure to ultraviolet radiation (UVR) deepens the pigmentation because it activates the melanocytes to produce more melanin.
Research is attempting to determine the roles of stem cell, neural, vascular and local hormonal factors in promoting melanocyte activation.
What Are The Clinical Features Of Melasma?
- Melasma presents as macules (freckle-like spots) and larger flat brown patches. These are found on both sides of the face and have an irregular border. There are several distinct patterns. It includes:
- Centrofacial pattern: forehead, cheeks, nose and upper lips
- Malar pattern: cheeks and nose
- Lateral cheek pattern
- Mandibular pattern: jawline
- Reddened or inflamed forms of melasma (also called erythrosis pigmentosa faciei)
- Poikiloderma of Civatte: Reddened, photoaging changes seen on the sides of the neck, mostly affecting patients older than 50 years.
- Brachial type of melasma affecting shoulders and upper arms (also called acquired brachial cutaneous dyschromatosis).
- Melasma is sometimes separated into epidermal (skin surface), dermal (deeper) and mixed types.
Epidermal Melasma
- Well-defined border.
- Dark brown color.
- Appears more obvious under black light.
- Responds well to treatment.
Dermal Melasma
- Ill-defined border.
- Light brown or bluish.
- Unchanged under black light.
- Responds poorly to treatment.
Mixed Melasma
- The most common type.
- Combination of bluish, light and dark brown patches.
- Mixed pattern seen under black light.
- Partial improvement with treatment.
